ACL Injury: Symptoms, Causes, And Treatments
We all have a friend, colleague, or family member who has torn their ACL and is considering a reconstruction. As physiotherapists, we are strong advocates for conservative management of injuries and will refrain from suggesting that you go under the knife 99% of the time. That being said, let’s explore the reasons why you should or shouldn’t consider surgery.
ACL tears are one of the most commonly seen injuries in sport and in our clinic. It is also one of the most researched orthopaedic conditions. Over the years, there has been an increasing push to investigate predisposing factors, methods and training modalities to prevent its occurrence.
What Is An ACL?
The Anterior Cruciate Ligament, also known as ACL, is a unique band of dense connective tissue that runs between your femur and tibia. The fibers travel inferiorly, medially, and anteriorly. Because of the orientation of its fibres, the ACL is commonly injured when there is a rotational force applied to the knee while it is bearing weight with a small amount of knee bending.
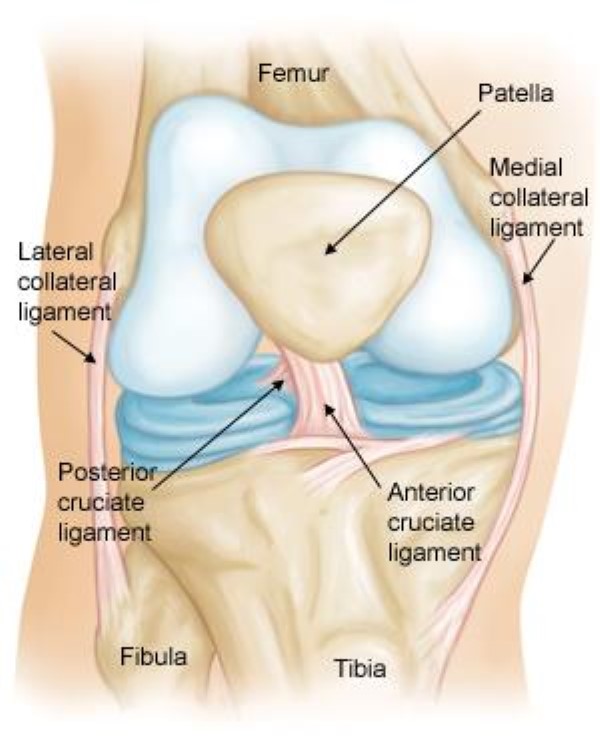
It functions as the primary restraint for anterior tibial translation and also restrains rotation at full knee extension.
The Mechanism Of ACL Injury
With its anatomy in mind, the most common mechanisms of injury are:
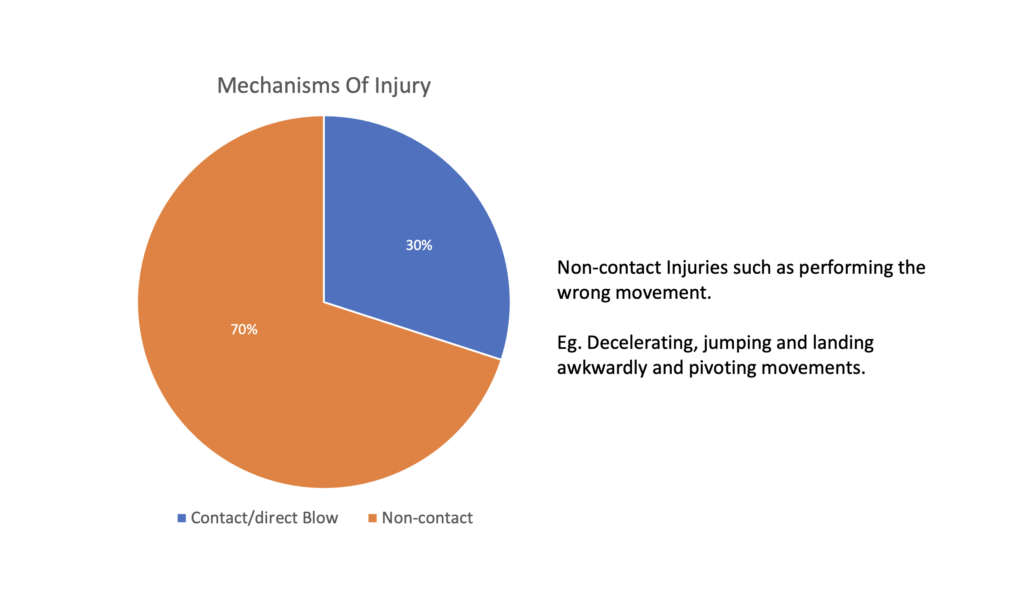
Some common non-contact ACL injury includes:
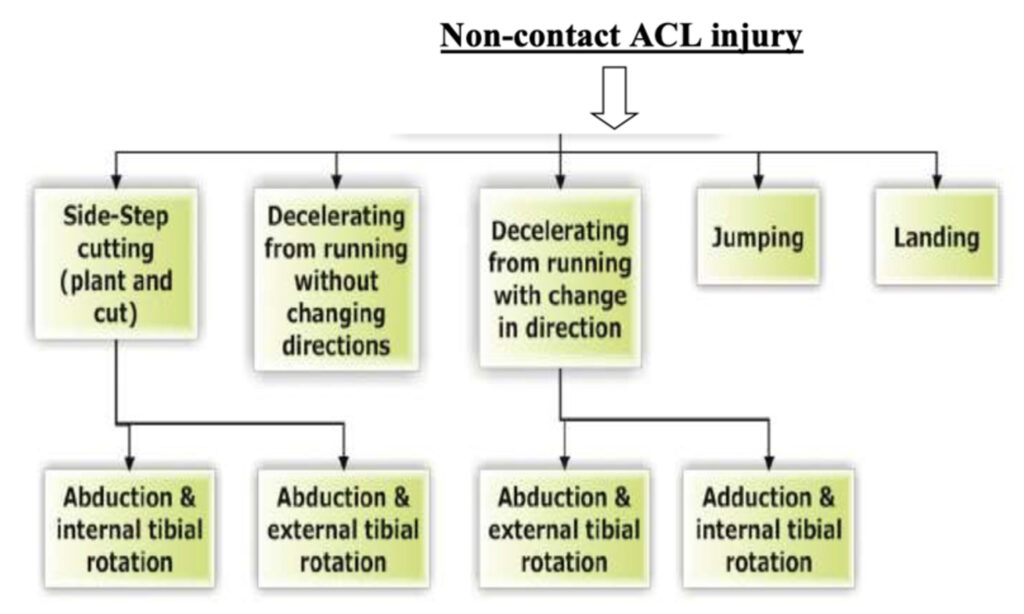
Signs And Symptoms Of An ACL Tear
Common signs and symptoms include:
- An audible ‘pop’
- Pain – May or may not be present depending on the severity of the tear. Often there is little to no pain with full rupture
- Swelling – It can take up to several hours after an incident (haemarthrosis)
- Instability or buckling of the joint under load
- Loss of range
Other predisposing factors include:
- Hormonal influence in females
- Sports that require frequent and sudden change in direction/pivoting (Eg. football, basketball, handball and gymnastics)
- Previous ACL injury
- Age
- Bony anatomy – Notch size, depth of tibial concavity
- Genetic predisposition
- Footwear
Do I Need To Undergo Surgery?
As physiotherapists, we are strong advocates for conservative management of injury. Through a thorough assessment and strengthening/stability program, you’ll be able to return to your activities of daily living with few residual deficits. People tend to underestimate how much effort and commitment is required to adhere to a post-op rehab program versus an activity modification and a comprehensive strengthening regime.
Unless you’re a high level athlete, have significant pain and structural compromise or participate in activities that require significant load and dynamic stability, the simple answer to your question is no. You don’t necessarily have to go under the knife.
We commonly see athletes opting very quickly for ACL reconstruction after injury and evidence suggests that in order to give your operation the best chance of success, a 6-8 week pre-hab exercise should be implemented. This allows you to develop the neuromuscular training, muscular strength and endurance to buffer the downtime you will experience post op. It allows you to essentially build a solid base of your pyramid before adding to it.
Surgery vs Physiotherapy
Several studies such as Frobell et al. (2010) demonstrated no significant benefit to early ACL reconstruction versus conventional rehab whereas Bergenson et al. (2022) compared early ACL intervention with later crossover and found a greater proportion of patients with early reconstruction reported acceptable knee function at 2, 5 and 10 years post-op.
To confuse everyone even more, recent evidence has emerged highlighting spontaneous recovery of fully ruptured ACLs with rehab and time alone with follow ups done at 2 and 5 years post injury (Filbay et al. 2022). While factors such as age, compliance with protocol, comorbidities/previous injury and training background should be considered, it certainly is promising!
What Should You Do If You Have An ACL Injury?
The amount of information we have access to is overwhelming and researching can often lead to more confusion. The best advice that anyone can follow is to always think long and hard about your goals and look at your current function.
Chat to your physiotherapist or orthopaedic surgeon to discuss the best way that you can work together to ensure the best outcome for your knee! The one thing all pieces of evidence agree on is that early intervention is key!
Written By: Nicola Ying, B.Sc. Sports Science (AUS), B.Sc. Biomedical Science (AUS), Doctor of Physiotherapy (AUS)
Nicola is an experienced Physiotherapist specialising in neurological and vestibular rehab, shoulder rehabilitation, and injury prevention. Formerly a competitive swimmer and footballer, she has found her new passion in martial arts and is an avid Muay Thai and Jiu-Jitsu practitioner. She also spends her free time advocating for sport inclusivity and disability awareness.
References:
- Bergerson E, Persson K, Svantesson E, et al. Superior Outcome of Early ACL Reconstruction versus Initial Non-reconstructive Treatment With Late Crossover to Surgery: A Study From the Swedish National Knee Ligament Registry. The American Journal of Sports Medicine. 2022;50(4):896-903. doi:10.1177/03635465211069995
- Brophy RH, Wojtys EM, Mack CD, Hawaldar K, Herzog MM, Owens BD. Factors associated with the mechanism of ACL tears in the National Football League: A video-based analysis. Orthopaedic journal of sports medicine. 2021 Nov 8;9(11):23259671211053301.
- Filbay S, Roemer F, Lohmander S, et al32 Spontaneous healing of the ruptured anterior cruciate ligament: observations from the KANON trialBMJ Open Sport & Exercise Medicine 2022;8:doi: 10.1136/bmjsem-2022-sportskongres.8
- Montalvo AM, Schneider DK, Yut L, et al“What’s my risk of sustaining an ACL injury while playing sports?” A systematic review with meta-analysisBritish Journal of Sports Medicine 2019;53:1003-1012.
- Takuma Kano, Takanori Kokubun, Kenji Murata, Yuichiro Oka, Kaichi Ozone, Kohei Arakawa, Yuri Morishita, Kiyomi Takayanagi & Naohiko Kanemura (2022) Influence of the site of injury on the spontaneous healing response in a rat model of total rupture of the anterior cruciate ligament, Connective Tissue Research, 63:2, 138-150, DOI: 10.1080/03008207.2021.1889529

